




Sciatica is a common yet debilitating condition that causes pain, tingling, or numbness radiating along the sciatic nerve.
For residents of Dubai, finding effective, long-term relief can be challenging, especially with treatment options often focusing on symptom management rather than the underlying causes.
As a McGill Method Certified Provider, I provide a science-based, non-invasive approach to sciatica treatment.
With evidence-based techniques developed by Dr. Stuart McGill, one of the world’s leading experts on low back pathologies, I help my clients alleviate pain, restore function, and build resilience against future flare-ups.
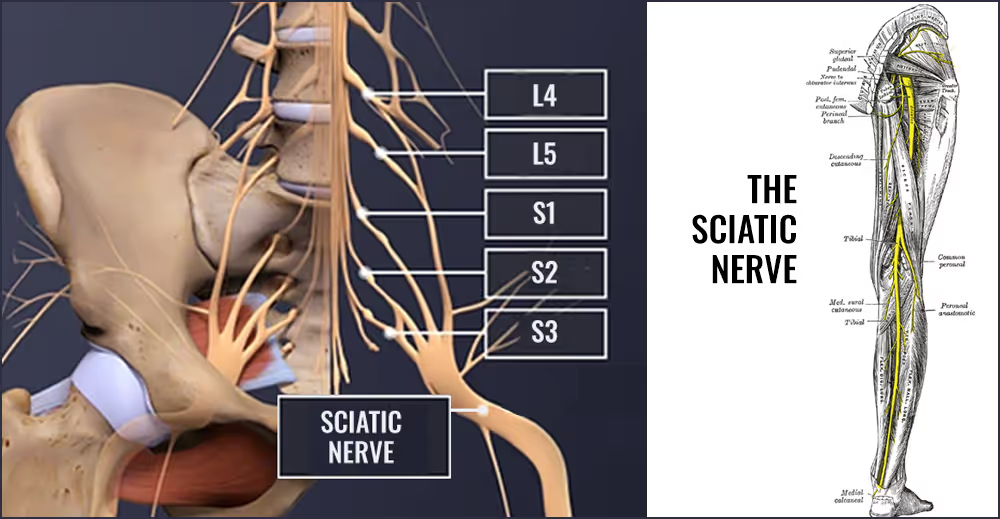
Understanding why sciatica occurs is key to treating it effectively. The majority of cases are linked to herniated discs at the L4-L5 and L5-S1 levels of the lumbar spine. These are among the more mobile spinal joints and they're also subjected to greater load due to their position at the base of the spine.
Forward bending, twisting, and improper lifting techniques place disproportionate stress on these discs making them more vulnerable to herniation.
When a disc herniates, its inner, gel-like nucleus can press against nearby nerve roots, such as the L4, L5, or S1 nerve roots, which are major contributors to the sciatic nerve. This compression or irritation can cause shooting pains down the back and side of the leg, sometimes reaching the foot or toes.
Disc herniation explained by Dr. Stuart McGill
Unlike many approaches that focus only on alleviating symptoms, the goal of the McGill Method is to identify your individual pain triggers, eliminate them from your daily routine, then build an injury-resistant back. It involves the following:
1. A Comprehensive Assessment
After taking a detailed personal history I take you through specific pain-provocation tests to pinpoint the exact causes of your sciatica. This allows us to identify the movements, postures, and loads that aggravate your pain and those that alleviate it.
2. The Elimination of Pain Triggers
Once we know what’s causing your sciatica, the first step is to remove your individual pain triggers from your daily life. I teach you personalised 'spine hygiene' which may involve adjusting how you sit, stand, lift, perform your daily activities and even sleep. This reduces stress on your damaged disc(s) which is essential to allow healing.
3. Building a Resilient Spine
Through precise exercises, we focus on rebuilding spinal stability, first via muscular endurance, then strength. Mobility of adjacent joints such as the hips may also need to be addressed in order to reduce stress on your spine. Your personalised exercise program is designed specifically for the level you're at now, and is progressed at regular intervals.
4. Progressive Rehabilitation
As your pain subsides, we gradually reintroduce more challenging movements to prepare your body for daily activities, sports, or work demands—whatever your goals may be.
Dubai offers numerous therapists and fitness professionals, but what sets me apart is my specialization in the McGill Method (I'm currently the only McGill Method certified practitioner based in Dubai). My unique expertise enables me to:
1. Empower you with knowledge about your condition and teach you how to manage it effectively.
2. Tailor a movement and exercise program specifically adapted to you as an individual.
3. Focus on long-term solutions instead of temporary pain relief.
Moreover, as a personal trainer based in Dubai, I understand the challenges of living in a fast-paced city where long hours, sedentary work, or intensive physical activities can exacerbate sciatica.
I’ll help you to adopt the movement and lifestyle habits that are required for a successful recovery.
 BOOK YOUR CONSULTATION
BOOK YOUR CONSULTATION
“I had been suffering from sciatica for two years. Despite seeing osteopaths and trying painkillers and exercises, I never managed to get rid of it permanently.
After working with Andy, not only did my sciatica disappear, but two years later it has never come back—even through pregnancy and after having a baby.”

“For several months I suffered from back and leg pain that made it impossible to sit or lie down without constantly shifting positions. Skeptical at first, I tried Andy’s approach of targeted postural exercises and reminders on proper movement.
Through patient, detailed sessions, Andy taught me how to move correctly and avoid harmful habits. Within weeks my back pain completely vanished.
His expertise and professionalism are unparalleled. I highly recommend his approach to anyone suffering from similar issues.
Thank you from the bottom of my heart for freeing me from pain!”
If you’re searching for sciatica treatment in Dubai, you don't need to settle for temporary fixes. I can help you regain control of your life with a proven, research-backed approach that treats the root cause of your pain.
Book a free consultation with me today to find out more.

“I call Andy a miracle worker. I suffered with chronic back pain for four years and tried everything: medication, physiotherapy, chiropractic care, acupuncture, massage, yoga. Nothing worked.
Remarkably, just by stopping the stretches I’d been doing for years, I experienced immediate relief.
Andy’s thorough approach and easy-to-follow program have made a huge difference. I now feel empowered, in control of my pain, and hopeful about the future. I understand my triggers and how to work around them.
Although there’s still a road ahead, I finally see a silver lining. I fully recommend working with Andy.”

“I started training with Andy because I wanted to get back to playing Padel regularly. For a long time, my lower back pain would stop me from playing as often as I wanted. I had been stretching for almost two years, but it never really solved the problem.
After working with Andy for about two months, I’ve noticed a big difference. I can now play without pain, I recover faster, and my core feels much stronger. The exercises he recommended made a real impact, and I finally understand what movements actually help my back instead of making it worse.
Andy really knows what he’s doing. He explains things clearly and focuses on long-term solutions rather than quick fixes. I’m going to continue with the program he gave me - it’s been a huge help.”

“I cannot recommend Andy highly enough! Despite being only 24, I suffered from poor posture, hours at the computer, and incorrect gym form—all of which led to a severe herniated disc.
After costly doctor visits, scans, and physical therapy with no relief, I turned to Andy. His knowledge and tailored approach helped me make a full recovery and safely resume resistance training. Andy’s support was truly priceless.
If you’re struggling with back pain, don’t hesitate to contact Andy—he genuinely is a miracle worker. Since my recovery, I have confidently referred several friends dealing with debilitating back pain to Andy.”

“I contacted Andy for the Low Back Pain Rehab Program in January 2024. Two years earlier I had injured my back (herniated disc), which led to chronic pain and fear of training again.
I came across Dr. Stuart McGill’s book, Back Mechanic, which helped, but I wanted personalized coaching. Andy’s at-home program included daily training, face-to-face sessions, and online follow-ups. He listened carefully and progressed my program safely.
Having recently completed it, I am now free of back pain, with greater core strength and resilience. I couldn’t be happier.
Thank you, Andy!”

“Andy was absolutely excellent. I’ve had back issues for years, and I’ve never felt better than after the program he arranged.
He showed me what I should do and also eliminated exercises I thought were helping but were actually harming me.
I cannot recommend him enough — super professional, accommodating, and with a personal approach!”

“After months of back pain and trying massages, stretching, yoga, and physiotherapy that only worsened my symptoms, I found Andy.
I was surprised how detailed and effective it was online. He quickly identified pain-causing movements and showed me how to modify them. The pain improved quickly and within weeks I was almost always pain-free.
Thank you for your patience and dedication, Andy. This money is well spent for the sake of a pain-free life.”

“Andy has worked a literal miracle on my back. Before, I had almost constant pain; now I hardly have any. His practical approach to strengthening, stretching, and movement comes from real experience and knowledge.
My general strength and fitness have also improved — I can run pain-free again. I couldn’t recommend him highly enough!”

“So glad I found The Back Coach. I struggled with back pain for years, including a herniated disc and pinched nerve.
After just a few weeks with Andy I made dramatic improvements. Six months later, I have virtually no pain and my core is stronger than it has been in years.
Thank you Andy!”

“How lucky to have found Andy! For several years I suffered from lumbar back pain, which worsened after pregnancy despite physiotherapy and exercise. I was starting to despair.
Andy's program saved me—I learned to relieve my pain, move correctly, restabilize my back, and build muscle. Andy’s professional follow-up and involvement, all by video, were simple and effective.
Thank you! I recommend him 100%.”

“I went to see Andy a few months ago after suffering my third or fourth incident of a disk bulge.
He showed me how to strengthen all the muscles around the lower back and core and I’m finally back in the gym and starting to lift weights again.
I couldn’t be happier. Andy has given me tools that I will use for the rest of my life to help me overcome back issues that no one else has been able to help me with.”

“I had been struggling with lower back pain (L4-L5) for almost three years. Surgery helped with leg pain but not the back pain itself.
I began Andy’s program four months ago with online sessions every two weeks. I now have days where I don’t notice my back at all and I’ve resumed ordinary activities I had stopped.
He is an extraordinary professional — always kind and willing to help. If he’s helped me this much in a few months, I can’t wait to see what’s next.
Thank you, Andy.”

“I was looking for a conservative way to manage lower back pain caused by a herniated disc. I found Andy through Instagram and began with a 3-hour assessment.
He created an 8-week program and met with me in person every two weeks to monitor progress and make changes. After following the program, my pain is now close to zero, my core is stronger, and my mobility has improved.
Andy also taught me subtle daily techniques — like how to pick things up or sit and stand without pain.
A true professional and expert in his field. Highly recommended.”

“I was in severe pain after a flare-up from a herniated disc. Andy helped me understand what was wrong and how to recover. He showed me how to move correctly in daily life, guided me through an extensive movement test and history, and gave me exercises to build endurance.
Even when I had setbacks, he helped me get back on track and understand why they happened. Very responsive and kind to work with. Thanks Andy!”

“I injured my back 6 years ago and have been dealing with chronic pain ever since. My case became complex and discouraging, but working with Andy has brought me back confidence and hope.
He has the skills I needed most: patience, understanding, and dedication. Chronic pain goes beyond the physical — it creates psychological insecurity — and Andy addressed both.
He is knowledgeable, notices subtle details that others miss, and prescribes the right exercises to improve not only my back but my overall condition.
Thank you very much, Andy.”

“After years of searching, Andy, The Back Coach has been the answer to my rehabilitation from a back injury. It’s a delight working with him.”

“After several disc bulge flare-ups in 2024, I found Andy while searching for Stuart McGill practitioners in Dubai. I’ve just completed a 9-week course with him and am very satisfied with my progress.
We began with a thorough assessment, then designed a program to get me moving again and rebuild core strength. As I improved, Andy added more exercises to build resilience.
His attention to detail and focus on proper form helped minimize the risk of further flare-ups.”