









I was talking to a German client of mine about how his mother tongue seems to have a word for everything. This reminded him of the word that came to his mind before he contacted me about his low back pain: Leidensdruck.
It roughly translates as: the 'pressure of suffering'. It's used when the level of discomfort and disruption to your life has finally reached a tipping point that forces you to change.
This is a common experience for people with chronic low back pain. But, waiting until you reach this point isn't always the wisest thing to do.
Not least, because of how the physiology of your spine works.
Your spine is no different from other parts of your body that when in distress don't send out warning signals until long after damage is done. The most obvious example is high blood pressure, caused by blood vessels staying too constricted and the body holding onto too much fluid, quietly damaging organs for years before you feel a thing.
Up to 42% of chronic low back pain is thought to be directly attributed to internal disruption of lumbar intervertebral discs (discogenic pain). And even when the disc isn’t the primary pain generator, degenerative disc changes often precede other common presentations (like radicular symptoms and facet joint pain).
But the bigger point is that structural 'wear-and-tear' findings are incredibly common on MRI. In one large study, 77.8% of people who reported back pain had at least one lumbar MRI finding (and 74.4% of people without back pain also had at least one).
That’s a lot of spinal degeneration, and not all of it causes pain. One reason for the high prevalence of disc degeneration in asymptomatic individuals is that it still hasn't reached the part of the disc that perceives pain.
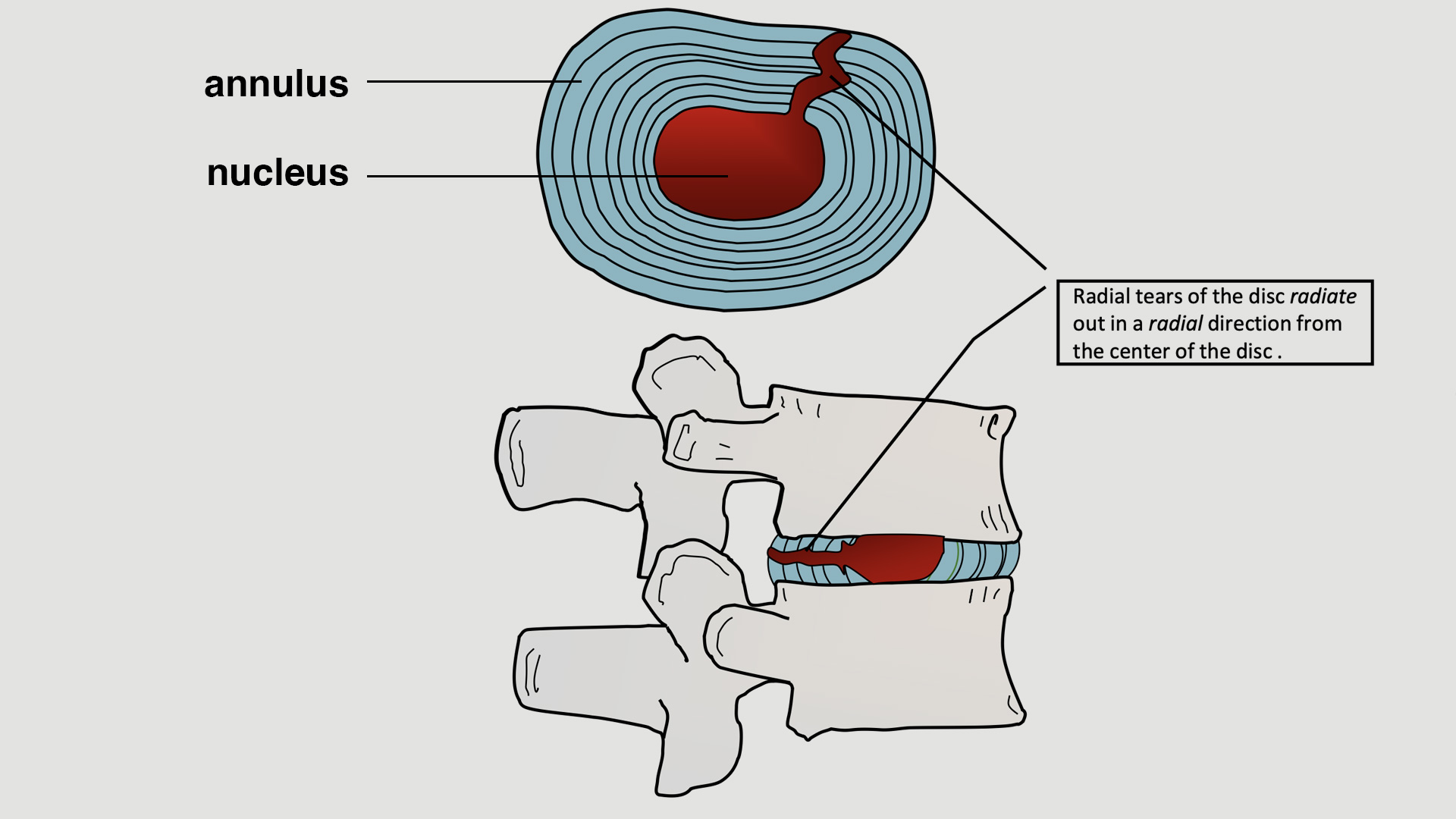
For example, a radial tear, which begins centrally and progresses outward in a radial direction, often causes little or no symptoms until it reaches the pain-sensitive, innervated outer layers of the disc annulus. Once it does, it can trigger discogenic pain, and may even allow inflammatory disc material from the nucleus to leak beyond the annulus and irritate or compress nearby nerves.
Picking up the pencil didn't cause your disc herniation. It was the preceding months or years of poor quality movement that did that. The pencil takes all the credit but, in reality, it only broke the final, thin line of defence that established contact with the nerves.
But, why would our spines suffer so much damage before sending out any pain signals?
Because while our intervertebral discs allow motion in our spines, they also have to absorb shock and sustain an enormous amount of compressive force, making them an inhospitable environment for the growth of nerves and blood vessels.
This has twofold consequences: we don't feel pain until the damage is already done. And once the damage is done, the lack of blood supply means that repair takes time and needs to be managed carefully.
A retrospective study (Hong 2016) found that most 'massive' lumbar disc herniations do, in fact, resolve (as indicated by MRI), but the timeframe varies widely: anywhere from 3 to 21 months.
More broadly speaking, we don't feel pain until significant damage is done to our discs for the same reason that we don't get warning signs about our high blood pressure until it's too late:
'We didn’t evolve to be healthy, but instead we were selected to have as many offspring as possible under diverse, challenging conditions.'
—Daniel Lieberman (The Story of the Human Body)
Evolution's priority of short-term survival strategies may also help to explain the unconscious compensation mechanisms that kick in to keep you functioning when you have a damaged disc in your spine. Your tight hip flexors or the muscle spasms in your QL (quadratus lumborum) are an emergency safety mechanism that attempt to stop you doing further damage to your spine but they're not an effective long term fix.
They're doing their best to give you another throw of the spear so you can to get your next meal and maybe get another chance to procreate this evening.
But, trying to stretch your symptoms away won't solve the underlying issue. That's invariably solved by learning how to move in a way that doesn't stress your spine and progressively building up its neglected muscular support system.
If you care about the condition of your spine from now until the end of your life (your spine has to last a lot longer now than it did before when we used to throw spears for a living), the smart move is not to wait until your Leidensdruck reaches its peak.