









Ali’s rehab didn't fix his back. It caused more degeneration. He'd been diagnosed with end plate damage and a disc bulge about a year before he came to see me.
His physical therapist had given him McKenzie-style 'floppy push-ups' (repeated prone back extensions, pictured above) to help his protruding disc 'migrate back into place.' That can be helpful for some people, but for others who have less than 70% of their original disc height, it can make matters worse due to excess spinal motion that irritates the facet joints.
This was the case with Ali. His disc bulge was significant, meaning it had lost almost 50% of its original height. He also has a 'type-A' personality which meant he took his rehab seriously, doing his prescribed exercises at least once a day, every day. More is always better, right?
Not in this case. He mistakenly believed that this would help him recover quicker and allow him to continue training MMA (Mixed Martial Arts) at the same time.
It didn't. Not only was his pain starting to get worse, it changed. Now he wasn't just intolerant of flexion. He had become intolerant of extension too - the floppy push-ups were becoming painful to execute.
His recent MRI showed facet joint arthropathy and a thickened ligamentum flavum: two common “next steps” in the classic degenerative cascade.
This “degenerative cascade” model has been described in classic spine literature as a progression through stages that begins with damage to the disc, then to the facet joints. Often this degeneration progresses further, resulting in in stenosis (a narrowing of the space surrounding the spinal nerves).
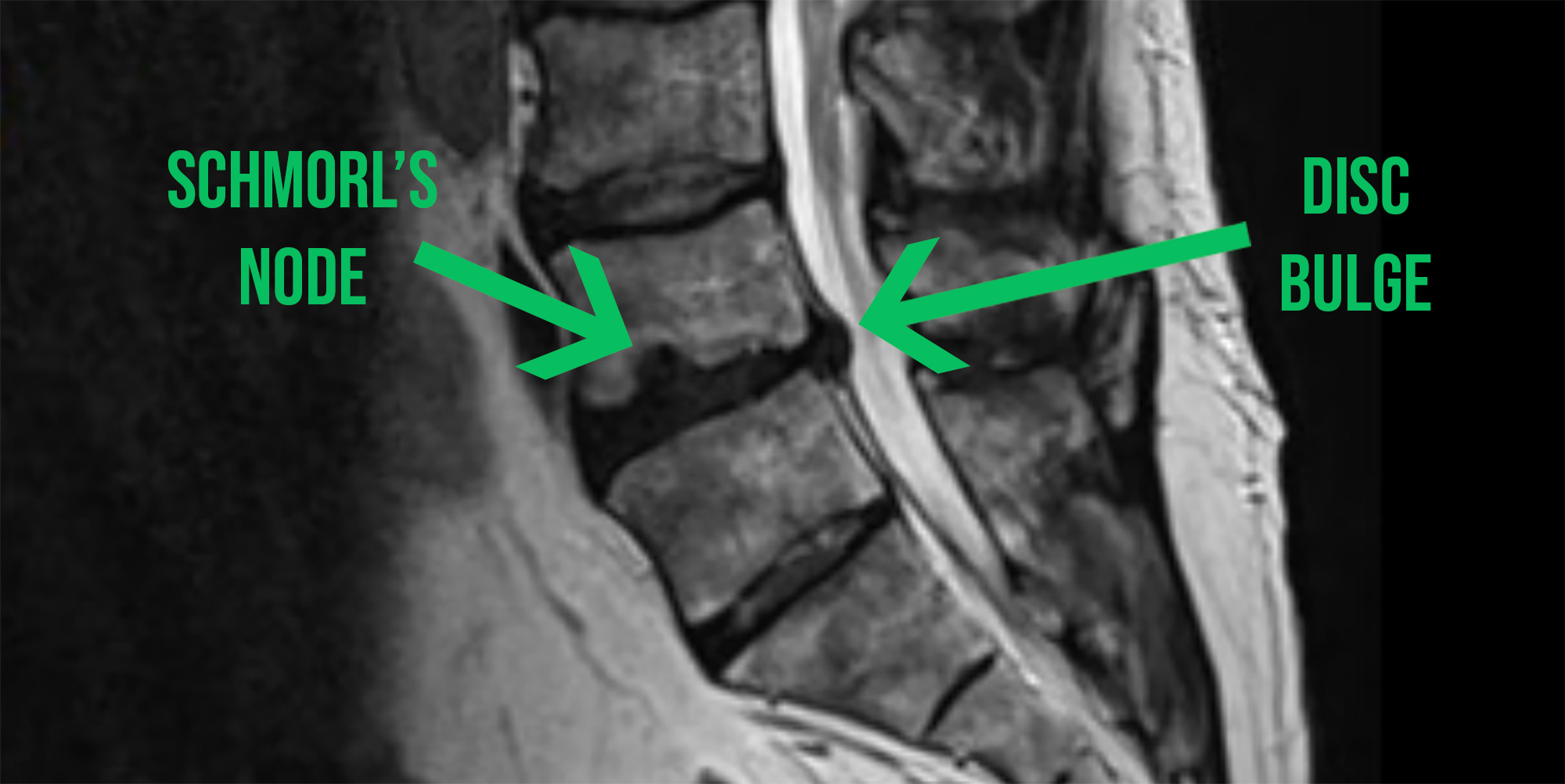
In young, healthy spines, the first part of the disc to get damaged is often the end plate (the superior or inferior interface of the disc with the vertebra which has a thickness of about half a millimetre). This occurs due to rapid compressive forces that occur in weightlifting, or in Ali's preferred sport, MMA.
This allows some of the nucleus of the disc to migrate into the vertebra above or below the disc (forming a Schmorl’s node), causing the joint to lose some of it's rigidity which alters the mechanics of the joint.
The resulting loss of joint stiffness can then lead to further damage of the passive joint tissues (discs and ligaments) which can result in a disc bulge or herniation.
It's a bit like letting some air out of one of the tyres on your car: it makes it harder to control and stabilise, which then increases wear and tear of the suspension.
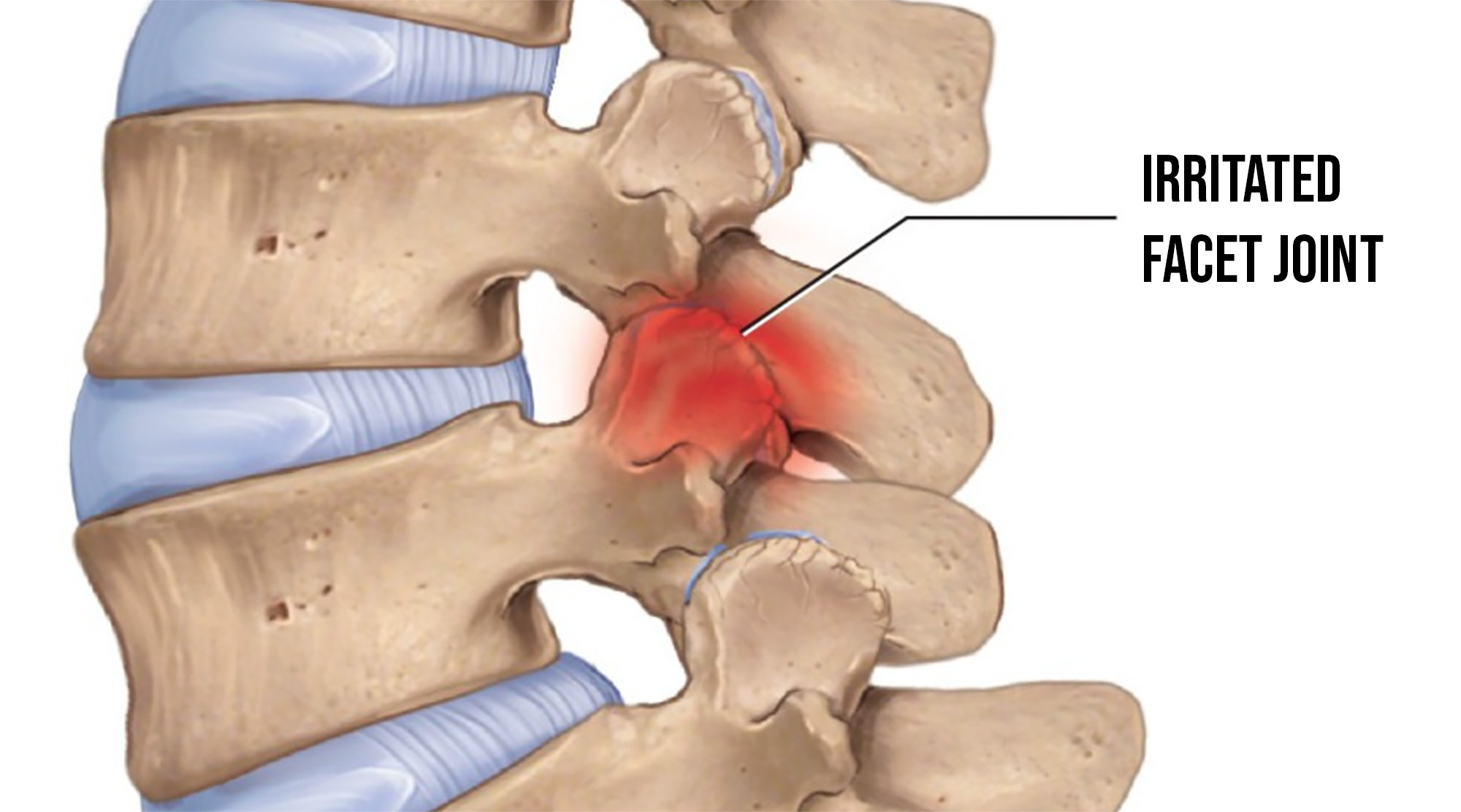
The facet joints are the small joints at the back of the spine. As disc mechanics change, those joints start to take more compressive stress and can develop arthritic changes over time (arthropathy). This is what was visible on Ali's recent MRI.
This is one reason some people get pain with standing, walking or arching. Upright positions often increase load on the facet joints in the posterior part of the spine.

“Stenosis” means narrowing. Degenerative lumbar stenosis is commonly linked to a combination of:
The “ligamentum flavum thickening” mentioned in Ali's MRI report is a well-recognised contributing factor to lumbar stenosis. It basically means there's even less space for the spinal nerves in an already crowded area.
This didn't appear to be the cause of Ali's current pain which would be rare at 25 years old. But, given these early signs at such a young age, the sensible thing to do would be to prevent further degenerative changes that result in disabling lumbar stenosis later in life.
The point of understanding the cascade isn’t to panic about the degenerative changes on your MRI. It’s to understand that you can prevent further degeneration (or at least slow it down considerably), by reducing the stress you direct through the damaged tissues in your spine.
Generic low back pain rehab exercises such as floppy push-ups are not the answer. The first step has to be a thorough assessment to determine what your individual pain triggers are, then develop a rehab plan around them.
This involves dialling back any activity that provokes your pain, or at least modifying your technique until your spine becomes less sensitised. In Ali's case, grappling and kicking were off the table because they were pain triggers, but he was able to carry on punching a bag because this didn't irritate his back.
Ali asked me what I thought about rhizolysis. This typically refers to radiofrequency ablation (RFA) of the medial branch nerves—the nerves that carry pain signals from the facet joints to the brain. It interrupts the pain signal, but doesn't prevent further degeneration.
In fact, when you no longer feel pain, it can be even more likely that further degeneration will occur because you can't feel the damage you're doing to an already vulnerable area.
Silencing the alarm without changing what’s triggering it can end up creating a bigger problem than you had to begin with.
This is why it's unlikely to be the best decision for a 25 year-old who plans to continue to compete in a high-load sport (although it may be the right decision for someone older who has already failed conservative approaches).
Once we removed the provocative loading, improved the endurance of Ali's spine-stabilising muscles, and moved around his triggers instead of through them, his pain settled and his function improved, allowing him to return to training.
Degeneration often progresses when pain is ignored, worked through or numbed. But when you identify what your spine tolerates, what it doesn’t, and train within those boundaries while gradually expanding them, the cascade can slow significantly.
So if your MRI mentions disc bulges, facet arthropathy, or early degenerative changes, you're not necessarily doomed to a life of back pain. You just need to learn how to move in a way that doesn't make the degeneration worse.